MSc Advanced Practice (Neonates)
- Course type
- Postgraduate
- Course qualification
- MSc
Course summary
What is the fee?
For all course options, see fees and funding
Where will I study?
Frederick Road campus
How long will I study?
One year
Overview
This practical course uses a work-based learning approach to develop the higher-level skills that lead to advanced practitioner status.
If you are an experienced neonatal intensive care nurse, this challenging and rewarding programme will enable you to become a qualified Advanced Neonatal Nurse Practitioner.
Pathway to Postgrad
Meet us in person at our Open Day to get a closer look at what studying here could mean for you. Or explore our other Pathway to Postgrad events taking place throughout June, with options to meet us online and on campus.
You will:
- Be supported in clinical practice by experienced neonatal nurse practitioners, consultant neonatologists, or specialist paediatric registrars.
- Be taught by experts in the field, including tertiary neonatologists, advanced neonatal nurse practitioners, midwifery lecturers, pharmacists, and radiographers.
- Develop advanced clinical skills in our simulation and skills suites with our award-winning human simulators.
- Have access to a clinical placement opportunity.
Course accreditations


This is for you if...
You are working in a neonatal unit with a minimum of five years of clinical experience.
You want to develop advanced clinical skills.
You are hardworking and dedicated to developing your knowledge.
The School of Health and Society

The School of Health and Society is a forward-thinking, dynamic school with a commitment to lifelong learning and real-world impact.
Our courses are informed by the latest research, and we work closely with organisations from both the public and private sector to ensure our teaching is at the forefront of practice. The University has received approval for a new health building on the Frederick Road campus which will create brand new teaching spaces, including new Podiatry spaces. Construction will begin in late 2024, with completion expected by Autumn 2026. This state-of-the-art facility will serve as a health and wellbeing hub, supporting popular healthcare courses and community services. It will feature sustainable design elements and provide modern clinical facilities to enhance student learning and community engagement. Find out more about our new Health Building.
In time community healthcare clinics will also take place there as partnerships are developed to explore research opportunities and to provide a range of therapeutic sessions.
Facilities

Clinical Practice Wards
Our Clinical Practice Wards are located in the Mary Seacole Building on the second floor. There are four rooms designed to provide the look and feel of a hospital environment. The rooms are furnished with patient beds, lockers, chairs, sinks, and curtains, as well as audio-visual equipment, internet, and a teaching area.
We also have several clinical skills rooms that enhance student learning, from taking blood pressure to giving CPR and more complicated procedures. Along with nursing skills rooms where you can practice in a ward situation, there are basic skills rooms for sessions such as moving and handling.
Simulation Suites
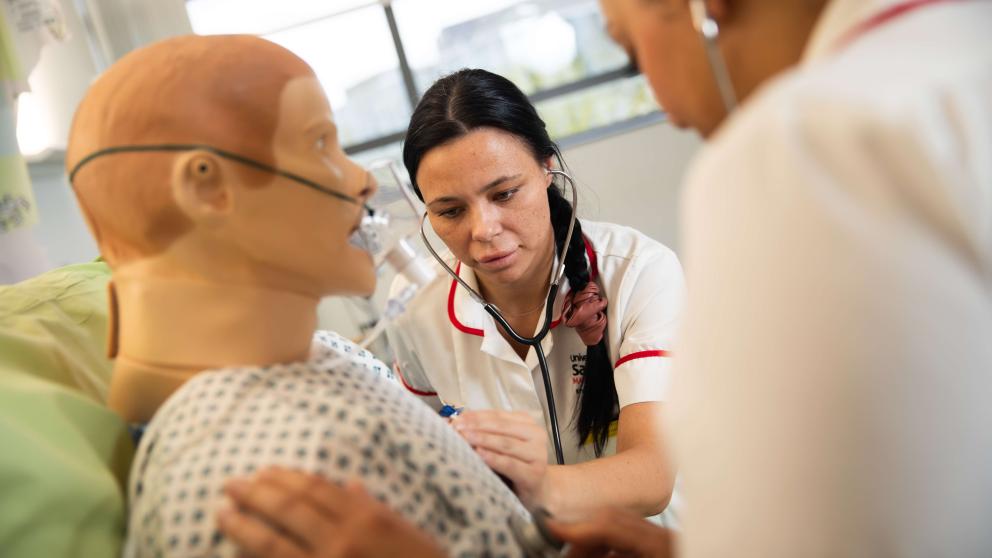
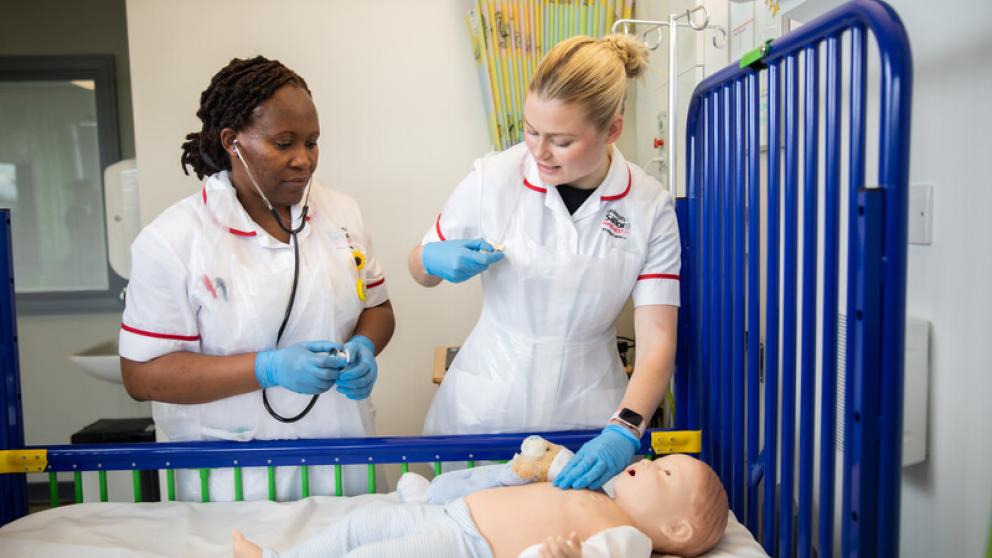
Our Simulation Suites provide you with the opportunity to tackle real-life scenarios in a safe and supported environment. Set up like a hospital ward, the lab contains hi-tech patient simulators that can mimic everything from the common cold to a major heart condition.
The equipment includes:
- Emergency Care Patient Simulators: Anatomically correct, feature-rich mannequins used for the physical demonstration of various clinical signs, including bleeding, breathing, blinking eyes, and convulsions.
- iStan Patient Simulators: A step up from the Emergency Care simulators, the iStan adds an essential human element to patient simulation. It moves, breathes, and can cry out or moan with pain, providing a realistic patient for you to practice on.
- Pedia Patient Simulator: A complete reproduction of a six-year-old child, enabling you to practice paediatric scenarios.
- Baby Simulator: This mannequin allows interaction with our most vulnerable patients in a safe, realistic learning environment.
All the simulation equipment can be linked to sophisticated computer and audio-visual aids. Groups of students can role-play a wide range of scenarios, with a lab coordinator observing, running, and intervening in the scenario remotely. Sophisticated computer equipment can also provide detailed physiological information for each of the simulators under observation. The lab will help you develop the clinical skills you need and the high-level communication skills that will make a real difference to your patients.
Teaching staff

Suzanne Threadgold
Suzanne is a full-time Neonatal Nursing Lecturer at the University of Salford. She is Programme Leader for the Advanced Practice Neonates programme and module leads Neonatal Practice A and Neonatal Practice B.
Suzanne’s clinical background is that she is a registered children’s nurse who qualified as an ANNP in 2017. She has been employed in neonatal intensive care units in the north-west and Thames Valley Neonatal Networks. Prior to becoming an ANNP her roles included Band 7 shift coordinator and Practice Development Sister. She is fortunate to have had exposure to the transport team and surgical neonatal care. Suzanne is a NLS instructor and has an interest in simulation.
Teaching staff

Sarah Fitchett
Sarah Fitchett is a full-time Neonatal Nursing Lecturer at the University of Salford. She module leads the Newborn and Infant Physical Examination (NIPE) and Quality in Specialty (QIS) modules for post-qualifying students.
With 25 years of neonatal nursing experience, Sarah is a registered nurse who has worked across all levels of neonatal units in the north-west. She has held roles such as Band 7 Coordinator and Practice Educator, leading the upskilling process during the transition of a neonatal unit from Level 2 to Level 3. Sarah has been actively involved in practice development for the North West Neonatal Network Educators and maintains strong links with the North West Neonatal Operational Delivery Network (ODN).
How you'll learn
Future careers
Upon completion of this course, students will become advanced neonatal nurse practitioners and will work on a medical rota. Some students may also wish to progress to a PhD or work as a nurse consultant or in a leadership role in clinical practice.
Further study
Further study may lead to PhD or Professional Doctorate level studies.
Career Links
There is an NHS-based clinical practice-dependent module, establishing close links with all the hospitals where advanced neonatal nurse practitioners (ANNPs) are placed.
Modules
This 12-month course requires a high level of commitment to succeed, and you will move from nursing to a medical rota immediately upon qualification.
You will achieve several clinical competencies, such as advanced resuscitation skills, insertion of percutaneous long lines, insertion of umbilical and venous catheters, airway management and intubation, and chest drains. Upon completion, you will be eligible for a non-medical advanced practitioner role in neonates, allowing you to work within a junior medical rota.
You are expected to be flexible during the programme to facilitate your learning and clinical practice/experience:
- During the first three months, you will be introduced to new concepts, theories, and medical management, including physiology and pathophysiology for neonates within the maternity department and Neonatal Intensive Care Unit.
- For the rest of the programme, you will attend university and work in clinical practice.
- You will self-roster your off-duty clinical practice/experience within your tertiary intensive neonatal care unit (learning on the job).
- You will be given a named supervisor (Consultant Neonatologist).
- You must accrue a minimum of 660 clinical hours during your twelve months of training.
- Simulation teaching will be undertaken in the University’s simulation suite and clinical areas.
The Non-Medical Prescribing module is accredited by the Nursing and Midwifery Council (NMC), Health and Care Professions Council (HCPC), and General Pharmaceutical Council (GPhC). Upon successful completion, you will be able to add an annotation to your professional registration as an independent prescriber. The programme is accredited by the Centre for Advancing Practice.
Year one
Neonatal Practice A
This module will include an advanced understanding of respiratory and cardiovascular system pathophysiology and management. You will review the examination of the newborn and clinical reasoning, including the NIPE module teaching and assessment.
Research Methods
This module will look at contemporary issues and debates in research as well as the design of research projects and developing research proposals.
Neonatal Practice B
You will study pathophysiology, gaining a deeper understanding of the physiology of abnormalities and how to manage these. You will also gain insight into different clinical conundrums.
Non-Medical Prescribing
Learn to evaluate and challenge prescribing practice with reference to evidence-based practice, equality and diversity, and clinical governance in a neonatal context.
Dissertation
You will also undertake a dissertation as the final component of the programme.
We take a flexible approach to our course delivery that promotes diversity and inclusivity and provides a blended learning experience, which will vary to meet specific programme requirements. This learning time includes formal lectures and interactive activities such as seminars, tutorials, practical sessions, laboratory and studio learning. Smaller classes may be used to support collaborative activities such as project and group work and presentations. A range of different assessments and feedback is offered to meet the needs of both our diverse student body and specific subject needs.
Our postgraduate taught courses are normally made up of 30 credit modules which are equal to 300 hours of learning time, or 15 credit modules which are equal to 150 hours of learning time. A Master’s degree typically comprises 180 credits, a PGDip 120 credits, and a PGCert 60 credits.
Entry requirements
Applicant profile
This course is designed for those working in a neonatal unit with a minimum of five years of clinical experience. To be accepted onto the programme, you will need a written agreement and clinical support from a nominated consultant neonatologist and your nurse line manager.
You will apply through the university’s general online application form. As part of the process, you will have a joint interview with your line manager, a consultant neonatologist, and a university lecturer. Funding arrangements will be agreed upon between your Local Trust and the University.
Standard entry requirements
Undergraduate degree
You will need to have a 2:1 degree in a relevant health-related area and work within a tertiary neonatal intensive care unit with a minimum of five years of clinical experience.
Anyone who does not have the required level of degree is advised to discuss their application with the Programme Leader; they may have the option of the Salford Alternative Entry Scheme (SAES) or Accreditation of Prior Certificated Learning (APCL) application route.
You will also need to possess the ENB 405/Quality in Specialty qualification and be live on the Nursing and Midwifery Council (NMC) register.
Alternative entry requirements
Salford Alternative Entry Scheme (SAES)
We welcome applications from students who may not meet the stated entry criteria but who can demonstrate their ability to pursue the course successfully. Once we have received your application we will assess it and recommend it for SAES if you are an eligible candidate.
There are two different routes through the Salford Alternative Entry Scheme and applicants will be directed to the one appropriate for their course. Assessment will either be through a review of prior learning or through a formal test.
To be considered for the Salford Alternative Entry Scheme you must have already achieved or be working towards GCSE Maths and English Grade C/4 (or equivalent).
Fees and funding
See fees below
2025/26
| Type of study | Fees |
|---|---|
| Full-time | £9,100 per year |
2026/27
| Type of study | Fees |
|---|---|
| Full-time | £9,360 per year |
2025/26
| Type of study | Fees |
|---|---|
| Full-time | £17,000 per year |
2026/27
| Type of study | Fees |
|---|---|
| Full-time | £17,520 per year |
Additional costs
You should consider additional costs which may include books, stationery, printing, binding and general subsistence on trips and visits.
How to apply
Still have some questions? Register for one of our Open Days or contact us:
By email: enquiries@salford.ac.uk
By phone: +44 (0)161 295 4545
