
PgCert Non-medical Prescribing and Enhanced Clinical Skills
- Course type
- Postgraduate
- Course qualification
- PgCert
Course summary
What is the fee?
For all course options, see fees and funding
Where will I study?
Frederick Road campus
How long will I study?
One year
Overview
This course offers registered nurses, pharmacists and allied health professionals (physiotherapists, podiatrists, paramedics and therapeutic radiographers) an opportunity to enhance their clinical skills and practice and become an independent non-medical prescriber. This increases your potential to access career opportunities and improves the service user/patient and carer experience by offering a timely and responsive access route to treatment.
This is a part-time course with two 30-credit modules starting in September or January. The delivery is a blended learning approach including taught blocks and online study - for both, there is a requirement for learning to take place within your own area of clinical practice.
- September start date commences with the Non-medical Prescribing module followed by Developing Clinical Skills (illness).
- January start date commences with Developing Clinical Skills (illness).
Pathway to Postgrad
Meet us in person at our Open Day to get a closer look at what studying here could mean for you. Or explore our other Pathway to Postgrad events taking place throughout June, with options to meet us online and on campus.
You will:
- Be taught by a multi-professional team of independent prescribers and clinical experts.
- Build the confidence to critically evaluate and challenge prescribing practice with reference to evidence-based practice, equality and diversity, and clinical governance.
- Create and implement innovative approaches to care delivery that meet the needs of your client group.
This is for you if...
You have a keen interest in improving patient care and access to treatment.
You want to develop skills to enhance patient care and increase timely access to treatment.
Learn to prescribe safely, appropriately, and cost-effectively as either a supplementary or an independent prescriber.
The School of Health and Society

The School of Health and Society is a forward-thinking, dynamic school with a commitment to lifelong learning and real-world impact.
Our courses are informed by the latest research, and we work closely with organisations from both the public and private sector to ensure our teaching is at the forefront of practice. The University has received approval for a new health building on the Frederick Road campus which will create brand new teaching spaces, including new Podiatry spaces. Construction will begin in late 2024, with completion expected by Autumn 2026. This state-of-the-art facility will serve as a health and wellbeing hub, supporting popular healthcare courses and community services. It will feature sustainable design elements and provide modern clinical facilities to enhance student learning and community engagement. Find out more about our new Health Building.
In time community healthcare clinics will also take place there as partnerships are developed to explore research opportunities and to provide a range of therapeutic sessions.
Facilities
Our Clinical Practice Wards are located in the Mary Seacole Building. There are four rooms designed to give the look and feel of a hospital environment. The rooms are furnished with patient beds, lockers, chairs, sinks, and curtains, as well as audio-visual equipment, internet, and a teaching area.
We also have a number of clinical skills rooms that enhance student learning, from taking blood pressure to giving CPR and performing more complicated procedures. Along with nursing skills rooms where you can practice in a ward situation, there are basic skills rooms for sessions such as moving and handling.
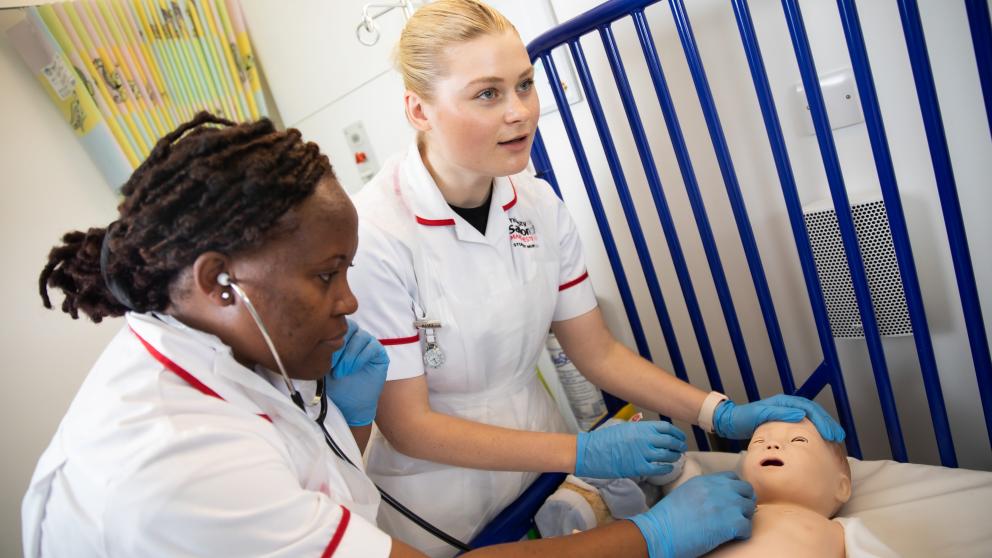
Patient Simulators
Our Simulation Suites provide you with the opportunity to tackle real-life scenarios in a safe and supported environment. Set up like a hospital ward, the Suites contain hi-tech patient simulators that can mimic everything from the common cold to a major heart condition.
The equipment includes:
- Emergency Care Patient Simulators: Anatomically correct, feature-rich mannequins, which can be used for the physical demonstration of various clinical signs including bleeding, breathing, blinking eyes, and convulsions.
- iStan Patient Simulators: A step up from the ECS, the iStan adds an essential human element to patient simulation. It moves, breathes, and can cry out or moan with pain, providing a realistic patient for you to practice on.
- Pedia Patient Simulator: A complete reproduction of a six-year-old child, enabling you to practice paediatric scenarios.
- Baby Simulator: This mannequin makes it possible to interact with our most vulnerable patients in a safe, realistic learning environment.
All the simulation equipment can be linked up to some very hi-tech computer and audio-visual aids. Groups of students get to role-play a wide range of different scenarios, with a lab coordinator observing, running, and intervening in the scenario remotely.
Sophisticated computer equipment can also provide detailed physiological information for each of the simulators under observation. The lab will help you develop the clinical skills you need, as well as the high-level communication skills that will make a real difference to your patients.
How you'll learn
Future careers
You may choose to pursue further study or use your enhanced clinical skills and non-medical prescribing qualification to progress in your chosen profession.
Career Links
We work with over 100 health and social care organisations so our links with industry are very strong. The successful completion of this programme enhances career opportunities for prescribing practice within all care sectors as it responds to an increased need for workforce development within the NHS.
Examples of job opportunities are increased employability within GP primary care for pharmacists and the substance misuse area of practice.
Modules
Teaching
You are taught through a combination of lectures, seminars and practice. Seminars are also used to enable you to discuss and develop your understanding of topics covered in lectures in smaller groups. In addition, you have timetabled meetings with your personal tutor.
- September start date commences with the Non-medical Prescribing module followed by Developing Clinical Skills (illness).
- January start date commences with Developing Clinical Skills (illness).
Independent learning
When not attending lectures, seminars and or other timetabled sessions you will be expected to continue learning independently through directed and self-study. Typically, this will involve reading journal articles and books, working on individual projects, undertaking research in the library, preparing coursework assignments and presentations, and preparing for examinations. Your independent learning is supported by a range of excellent facilities, including the library, the learning zone, and our computer learning zones. For NMP you will also have access to an e-learning interactive website.
Modules
Developing Clinical Skills (illness)
During this module you will explore:
- Advancing practitioner roles
- Planning, implementing and evaluating patient care
- Legal and ethical principles
- Strategies for knowledge and skill acquisition
- Local health issues
This module will build on your current skills and knowledge in order to create and implement new approaches to care to deliver that meets the needs of your client group. This module starts in January.
Non-Medical Prescribing
During this module you will explore:
Consultation, decision-making and therapy, including referral
- Influences on, and psychology of, prescribing
- Prescribing in a team context
- Clinical pharmacology, including the effects of co-morbidity
- Evidence-based practice and clinical governance in relation to non-medical prescribing
- Principles and methods of monitoring response to therapy
- Legal, policy and ethical aspects
- Professional standards, accountability and responsibility
- Prescribing in the public health context
- Portfolio development
This module is accredited by the NMC, HCPC and GPhC and upon successful completion, you will be able to add an annotation to your professional registration as an independent prescriber.
This module starts in September.
We take a flexible approach to our course delivery that promotes diversity and inclusivity and provides a blended learning experience, which will vary to meet specific programme requirements. This learning time includes formal lectures and interactive activities such as seminars, tutorials, practical sessions, laboratory and studio learning. Smaller classes may be used to support collaborative activities such as project and group work and presentations. A range of different assessments and feedback is offered to meet the needs of both our diverse student body and specific subject needs.
Our postgraduate taught courses are normally made up of 30 credit modules which are equal to 300 hours of learning time, or 15 credit modules which are equal to 150 hours of learning time. A Master’s degree typically comprises 180 credits, a PGDip 120 credits, and a PGCert 60 credits.
Please note that exact modules and content offered may vary in order to keep content current and, for courses that offer optional modules, may depend on the number of students selecting particular options. When accepting your offer of a place to study on a programme with optional modules, you should be aware that optional modules may not all run each year. Your tutor will be able to advise you as to the available options on or before the start of the programme. Whilst the University tries to ensure that you can undertake your preferred options, it cannot guarantee this.
Entry requirements
Applicant profile
The General Entry Academic Requirements are as per the university’s Admissions and Retention Policy detail for Postgraduate Taught Programmes.
Nurses and Allied Health Professionals applying to this module should have three years post-registration experience. Pharmacists require two years of post-registration experience.
Identification of a DMP (Designated Medical Practitioner) This must be a doctor who meets the criteria to supervise a trainee NMP and has agreed to undertake the role.
For clinical skills, you will need:
- Line managers support for work-based supervision and assessment of clinical skills agreed through a tripartite learning agreement
- A practice-based supervisor and assessor to facilitate the development of clinical skills
For your work-based placements:
For Non-Medical Prescribing, you will need to identify a DMP (Designated Medical Practitioner). For nurses, this can be either a doctor or a suitably experienced qualified prescriber acting as a practice assessor. This must be a doctor or suitably qualified independent prescriber who meets the criteria set by the professional regulatory bodies to supervise a trainee NMP and has agreed to undertake the role.
You will also need:
A practice-based supervisor and assessor to facilitate the development of clinical skills.
Applications and funding:
For the Non-Medical Prescribing Module only:
If you are self-funding, please complete a university application form as well as the application form on the Health and Education Cooperative website.
NHS employees may be eligible for a funded place. The NMP Lead within your organisation or training hub will be able to provide further information. If you are unsure of who to contact please contact the programme leader at the University of Salford, Jill Bentley j.bentley3@salford.ac.uk
For application enquiries contact Maria Pavlakou and to submit completed applications to healthsociety-nonmedicalprescribing@salford.ac.uk
For course enquiries, please contact Jill Bentley at j.bentley3@salford.ac.uk
Pharmacist self-funding/employed entry criteria enquiries and pharmacist-specific enquiries, please contact our pharmacist Clare Liptrott at c.liptrott@salford.ac.uk
Standard entry requirements
Undergraduate degree
You should have an undergraduate degree in a related discipline and be a registered health care professional such as a nurse, midwife, podiatrist, physiotherapist, paramedic and pharmacist.
Nurses or midwives should have one year of post-registration experience
Allied Health Professionals should have three years post-registration experience.
Pharmacists are required to meet the GPhC standards for entry onto prescribing programmes and be able to demonstrate:
- relevant experience in a UK pharmacy setting
- the ability to recognise, understand and articulate the skills and attributes required by a prescriber, and
- an identified area of clinical or therapeutic practice
GCSE
Applicants must have the equivalent of a grade C or above, GCSE Mathematics and GCSE English.
Subject specific requirements
Current professional registration with GPhC, NMC or HCPC.
Alternative entry requirements
Salford Alternative Entry Scheme (SAES)
We welcome applications from students who may not meet the stated entry criteria but who can demonstrate their ability to pursue the course successfully. Once we have received your application we will assess it and recommend it for SAES if you are an eligible candidate.
There are two different routes through the Salford Alternative Entry Scheme and applicants will be directed to the one appropriate for their course. Assessment will either be through a review of prior learning or through a formal test.
To be considered for the Salford Alternative Entry Scheme you must have already achieved or be working towards GCSE Maths and English Grade C/4 (or equivalent).
Fees and funding
On completion, there is a fee for annotation of your independent prescribing qualification to your professional registration. Please check with your professional body regarding cost.
2025/26
| Type of study | Fees |
|---|---|
| Part-time | £1,540 per 30 credit module |
2026/27
| Type of study | Fees |
|---|---|
| Part-time | £1,580 per 30 credit module |
How to apply
Still have some questions? Register for one of our Open Days or contact us:
By email: enquiries@salford.ac.uk
By phone: +44 (0)161 295 4545
